Alopecia
What is Alopecia?
Alopecia is a general term for hair loss. It can have different causes and types, such as autoimmune, genetic, or mechanical. Alopecia can affect the scalp or other parts of the body.
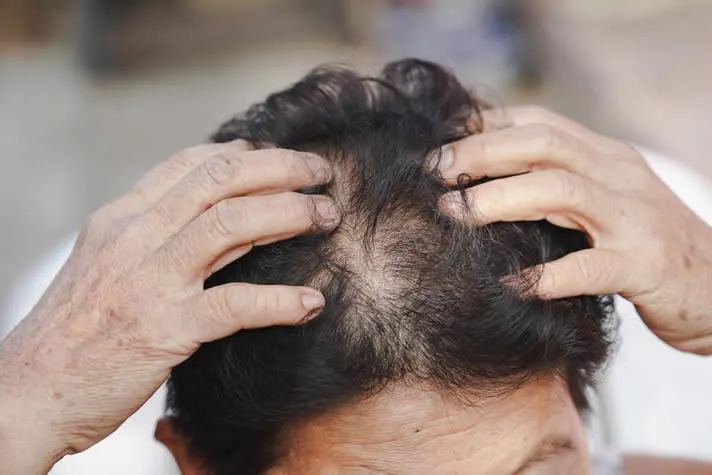
What are the signs and symptoms of Alopecia?
Gradual thinning of the hair on the top of the head. This is the most common type of hair loss, affecting people as they age. It may affect men or women differently. Patchy or circular bald spots on the scalp, beard, eyebrows, or eyelashes. This may indicate alopecia areata, an autoimmune condition that causes hair loss in small areas. The skin may be itchy or painful before the hair falls out. Sudden loosening of hair due to physical or emotional stress. This may cause overall hair thinning or hair loss in large clumps. Full-body hair loss due to certain medical treatments, such as chemotherapy or radiation therapy. The hair usually grows back after the treatment is over. Scaling, redness, swelling, or oozing on the scalp. This may indicate a fungal infection, such as ringworm, or a skin condition, such as psoriasis or seborrheic dermatitis.
What are the causes of Alopecia?
The causes of alopecia may vary depending on the type and cause of hair loss. Some common causes are:
- Autoimmune disease: This is when the immune system mistakenly attacks the hair follicles, causing hair loss in patches or all over the body. This is the cause of alopecia areata, which may be triggered by stress, illness, or genetic factors.
- Genetic and hormonal factors: This is when the hair follicles are affected by inherited genes or changes in hormones, such as during puberty, pregnancy, or menopause. This is the cause of androgenetic alopecia, also known as male or female pattern hair loss.
- Excessive pulling or tension on the hair: This is when the hair is damaged by hairstyles that pull the hair too tight, such as braids, cornrows, or extensions. This can lead to inflammation and scarring of the scalp, causing permanent hair loss. This is the cause of traction alopecia.
- Medical treatments or conditions: This is when the hair is affected by drugs, such as chemotherapy or radiation therapy, that cause hair loss as a side effect. The hair usually grows back after the treatment is over. Other medical conditions that can cause hair loss include thyroid disease, iron deficiency, fungal infections, or skin diseases.
What treatments are available at the dermatologist for Alopecia?
- Corticosteroid injections: This is a common treatment for alopecia areata, an autoimmune condition that causes patchy hair loss. The dermatologist injects a medication into the bald areas to suppress the immune system and stimulate hair growth.
- Minoxidil: This is an over-the-counter medication that comes in liquid, foam, or shampoo forms. It can help slow down or stop hair loss and promote hair regrowth.
- Finasteride: This is a prescription medication for men with androgenetic alopecia, also known as male pattern hair loss. It works by blocking the hormone that causes hair follicles to shrink and stop producing hair
- Hair transplantation: This is a surgical procedure that involves moving hair follicles from one part of the scalp to another where there is hair loss. It can be used to treat various types of alopecia, such as androgenetic alopecia, traction alopecia, or scarring alopecia.
- Laser therapy: This is a noninvasive treatment that uses low-level laser light to stimulate blood flow and cellular activity in the scalp. It can help improve hair density and quality in people with androgenetic alopecia or alopecia areata.

What are the different types of Alopecia and how are they diagnosed?
Alopecia is a general term for hair loss. There are different types of alopecia, such as androgenetic alopecia, alopecia areata, traction alopecia, and cicatricial alopecia. They are diagnosed by a dermatologist through a physical examination and medical history. Sometimes, a biopsy or other tests may be needed to confirm the diagnosis or rule out other causes of hair loss.
FAQ About Alopecia
What are the treatment options and home remedies for alopecia?
Some possible treatment options and home remedies for alopecia are Medications,Surgery,Laser therapy & Some natural or herbal remedies may help improve the health of the scalp and hair
What are some tips to prevent or reduce hair loss?
Avoid hairstyles that pull the hair too tight, Use gentle hair products and avoid harsh chemicals, Wash and condition your hair regularly, Dry your hair gently and avoid excessive heat styling, Eat a balanced diet and take supplements if needed & Manage your stress levels and get enough sleep.
What are some myths and misconceptions about alopecia?
There are different types of alopecia, such as alopecia areata, androgenic alopecia, and cicatricial alopecia. Alopecia can affect anyone, regardless of age, gender, or ethnicity. However, there are also many myths and misconceptions about alopecia that can lead to confusion and stigma
Is there a dermatologist near me in Richmond that offers treatment for alopecia?
Yes. At our Richmond dermatology office we offer treatment for alopecia to patients from Richmond and the surrounding area. Contact our office today to schedule an appointment.